- Your cart is empty
- Continue Shopping
Product
- Canaan Pharmacy Online Pharmacy | Online Canadian Pharmacy
- Need More Information Call Us 1-833-356-6337
Product description
INDICATIONS
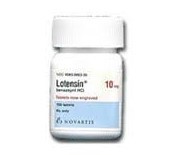
Lotensin is used for treating high blood pressure. It may be used alone or with other blood pressure medicines. Lotensin is an angiotensin-converting enzyme (ACE) inhibitor. It works by decreasing a chemical that tightens blood vessels. This causes the blood vessels to relax (dilate), which lowers blood pressure.
INSTRUCTIONS
Use Lotensin as directed by your doctor.
- Take Lotensin by mouth with or without food.
- Taking Lotensin at the same time each day will help you remember to take it.
- Drink plenty of fluids while taking Lotensin. Not drinking enough fluids or excessive sweating, diarrhea, or vomiting can lead to lightheadedness or fainting.
- If you miss a dose of Lotensin, take it as soon as possible. If it is almost time for your next dose, skip the missed dose and go back to your regular dosing schedule. Do not take 2 doses at once.
Ask your health care provider any questions you may have about how to use Lotensin.
STORAGE
Store Lotensin at or below 86 degrees F (30 degrees C). Store away from heat, moisture, and light. Do not store in the bathroom. Keep Lotensin out of the reach of children and away from pets.
MORE INFO:
Active Ingredient: Benazepril hydrochloride.
Safety information
Do NOT use Lotensin if:
- you are allergic to any ingredient in Lotensin or to any other ACE inhibitor (eg, lisinopril)
- you have a history of angioedema (eg, swelling of the hands, face, lips, eyes, throat, or tongue; difficulty swallowing or breathing; or hoarseness)
- you are pregnant.
Contact your doctor or health care provider right away if any of these apply to you.
Some medical conditions may interact with Lotensin. Tell your health care provider if you have any medical conditions, especially if any of the following apply to you:
- if you are pregnant, planning to become pregnant, or are breast-feeding
- if you are taking any prescription or nonprescription medicine, herbal preparation, or dietary supplement
- if you have allergies to medicines, foods, or other substances
- if you have or have ever had liver or kidney problems, kidney transplantation, or diabetes
- if you have systemic lupus erythematosus (SLE or lupus), scleroderma or a collagen vascular disease (ask your doctor if you are not sure), bone marrow suppression, low blood counts, low blood pressure, low blood sodium, high blood potassium, or narrowing or hardening of the arteries of the brain, or if you are dehydrated
- if you are scheduled to have surgery or to receive anesthesia or kidney dialysis.
Some medicines may interact with Lotensin. Tell your health care provider if you are taking any other medicines, especially any of the following:
- Dextran sulfate or thiazide diuretics (eg, hydrochlorothiazide) because the risk of serious damage to the kidney (eg, decreased urine output, weight gain) may be increased
- Lithium because the risk of toxic side effects (eg, tiredness; confusion; slurred speech; muscle tremors, spasms, weakness, or involuntary movements; seizures; loss of consciousness; coma) may be increased by Lotensin
- Indomethacin because it may decrease Lotensin’s effectiveness
- Insulin or oral diabetes medicine (eg, glyburide) because the risk of side effects, including low blood sugar levels (eg, hunger, shakiness or weakness, dizziness, headache, sweating), may be increased by Lotensin
- Potassium-sparing diuretics (eg, amiloride) or potassium supplements because the risk of side effects, including high blood potassium levels resulting in listlessness, confusion, abnormal skin sensations of the arms and legs, heaviness of limbs, slow or irregular heartbeat, or stopping of the heart, may be increased
- Certain gold-containing medicines (eg, sodium aurothiomalate) because flushing, nausea, vomiting, and low blood pressure may occur
- Thiopurines (eg, azathioprine) because the risk of their side effects (eg, a low white blood cell count, increase in infections) may be increased by Lotensin.
This may not be a complete list of all interactions that may occur. Ask your health care provider if Lotensin may interact with other medicines that you take. Check with your health care provider before you start, stop, or change the dose of any medicine.
Important safety information:
- Lotensin may cause drowsiness, dizziness, or lightheadedness. These effects may be worse if you take it with alcohol or certain medicines. Use Lotensin with caution. Do not drive or perform other possible unsafe tasks until you know how you react to it.
- Lotensin may cause dizziness, lightheadedness, or fainting; alcohol, hot weather, exercise, or fever may increase these effects. To prevent them, sit up or stand slowly, especially in the morning. Sit or lie down at the first sign of any of these effects.
- Patients who take medicine for high blood pressure often feel tired or run down for a few weeks after starting treatment. Be sure to take your medicine even if you may not feel “normal.” Tell your doctor if you develop any new symptoms.
- Lotensin may cause a dry, unproductive cough. This symptom usually stops after treatment with Lotensin is stopped.
- Tell your doctor or dentist that you take Lotensin before you receive any medical or dental care, emergency care, or surgery.
- Check with your doctor before you use a salt substitute or a product that has potassium in it.
- Diabetes patients – Lotensin may affect your blood sugar. Check blood sugar levels closely. Ask your doctor before you change the dose of your diabetes medicine.
- Lab tests, including blood pressure, may be performed while you use Lotensin. These tests may be used to monitor your condition or check for side effects. Be sure to keep all doctor and lab appointments.
- Lotensin should not be used in children younger than 6 years old; safety and effectiveness in these children have not been confirmed.
- Pregnancy and breast-feeding: Lotensin may cause fetal and newborn death if you take it while you are pregnant. If you think you may be pregnant, contact your doctor right away. Lotensin is found in breast milk. Do not breastfeed while taking Lotensin.
Side effects
All medicines may cause side effects, but many people have no, or minor, side effects.
Check with your doctor if any of these most common side effects persist or become bothersome:
Cough; dizziness, especially when standing; headache; nausea; sleepiness; tiredness.
Seek medical attention right away if any of these severe side effects occur:
Severe allergic reactions (rash; hives; itching; difficulty breathing; tightness in the chest; swelling of the mouth, face, lips, or tongue); chest pain; chills; fainting; fever; hoarseness; irregular or slow heartbeat; lightheadedness; sore throat; unusual stomach pain; yellowing of the skin or eyes.
This is not a complete list of all side effects that may occur. If you have questions about side effects, contact your health care provider.
Need More Information? Call Us Toll Free: 1-833-356-6337
| Package | 10mg × 60 pills, 10mg × 90 pills, 10mg × 120 pills, 10mg × 180 pills, 10mg × 270 pills, 10mg × 360 pills |
|---|